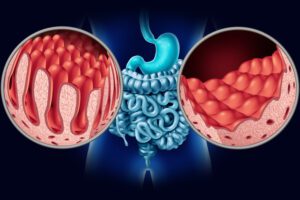
Black people with celiac disease have an increased risk of not being diagnosed
Physicians' common view that celiac disease is rare in Black Americans can lead to disparity in testing for the condition, according to the study, published recently as a research letter in the journal, Gastro Hep Advances.