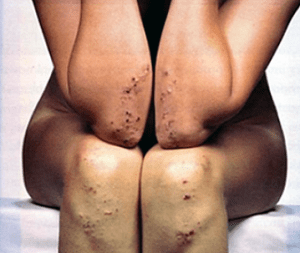
 Dermatitis herpetiformis (DH) is a severe, chronic skin rash associated with celiac disease.
Dermatitis herpetiformis (DH) is a severe, chronic skin rash associated with celiac disease.
The symptoms of dermatitis herpetiformis are extremely itchy and blistering skin. Sometimes referred to as gluten rash or celiac rash, DH is a chronic condition that is considered to be the skin form of celiac disease. Not all people with celiac disease develop DH, but most people with DH have celiac disease.
The rash usually occurs on the elbows, knees, and buttocks and it is typically symmetrical, meaning it appears on both sides of the body. When this gluten-related rash goes away, which it often does spontaneously, it may leave brown or pale marks on the skin where pigmentation is lost.
DH is commonly mistaken for other conditions such as:
In the past, DH was also known as Duhring disease, Duhring-Brocq disease or Brocq-Duhring disease.
Only about 20 percent of people with DH have intestinal symptoms of celiac disease, however, biopsies show that 80 percent have some degree of damage to the small intestine, especially if a high gluten diet is maintained.
DH is a skin manifestation of celiac disease and is part of the abnormal immune response to gluten. For those with celiac disease and DH, eating gluten triggers an autoimmune response which causes DH blisters to form. This rash is connected to celiac disease, not non-celiac gluten sensitivity (‘gluten sensitivity’).
Dermatitis herpetiformis symptoms include:
It can appear anywhere on the body but most frequently appears on the elbows, knees, buttocks, lower back and scalp. Doctors diagnose dermatitis herpetiformis by performing a biopsy on the cells under the top layer of skin.
Learn more about dermatitis herpetiformis symptoms and testing.
Dermatitis herpetiformis treatment consists of a lifelong gluten-free diet, just like celiac disease. It may take about six months to achieve some improvement in the skin condition and up to two years or more to get total control through the gluten-free diet alone. Additionally, Rash symptoms can be controlled with dapsone, an antibacterial medication.
Learn more about dermatitis herpetiformis treatment.
Read patient stories, and access links to research and other resources.
Do you or a family member suspect dermatitis herpetiformis? You may have celiac disease. Find out now: take our Celiac Disease Symptoms Checklist and reach out to your doctor.
Opt-in to stay up-to-date on the latest news.
Yes, I want to advance research No, I'd prefer not to